Diabetologist Anoop Misra, who had been treating a 30-year-old for obesity with the weight-loss injectable drug tirzepatide (sold as Mounjaro), was surprised when the latter didn’t lose as much weight. “He had been on the medication for about two months but I didn’t see the change I expected despite a third dose escalation,” says the chairman of Fortis C-DOC Hospital for Diabetes and Allied Sciences, New Delhi.
Speaking about his non-responder patient with The Indian Express, Dr Misra says, “The patient began questioning the drug after hearing that a particular pharmacy might be dispensing fake drugs. While I dismissed his fears, saying such claims could be untrue, the lack of expected weight loss was concerning. This was my first patient who had reported such an anomaly.”

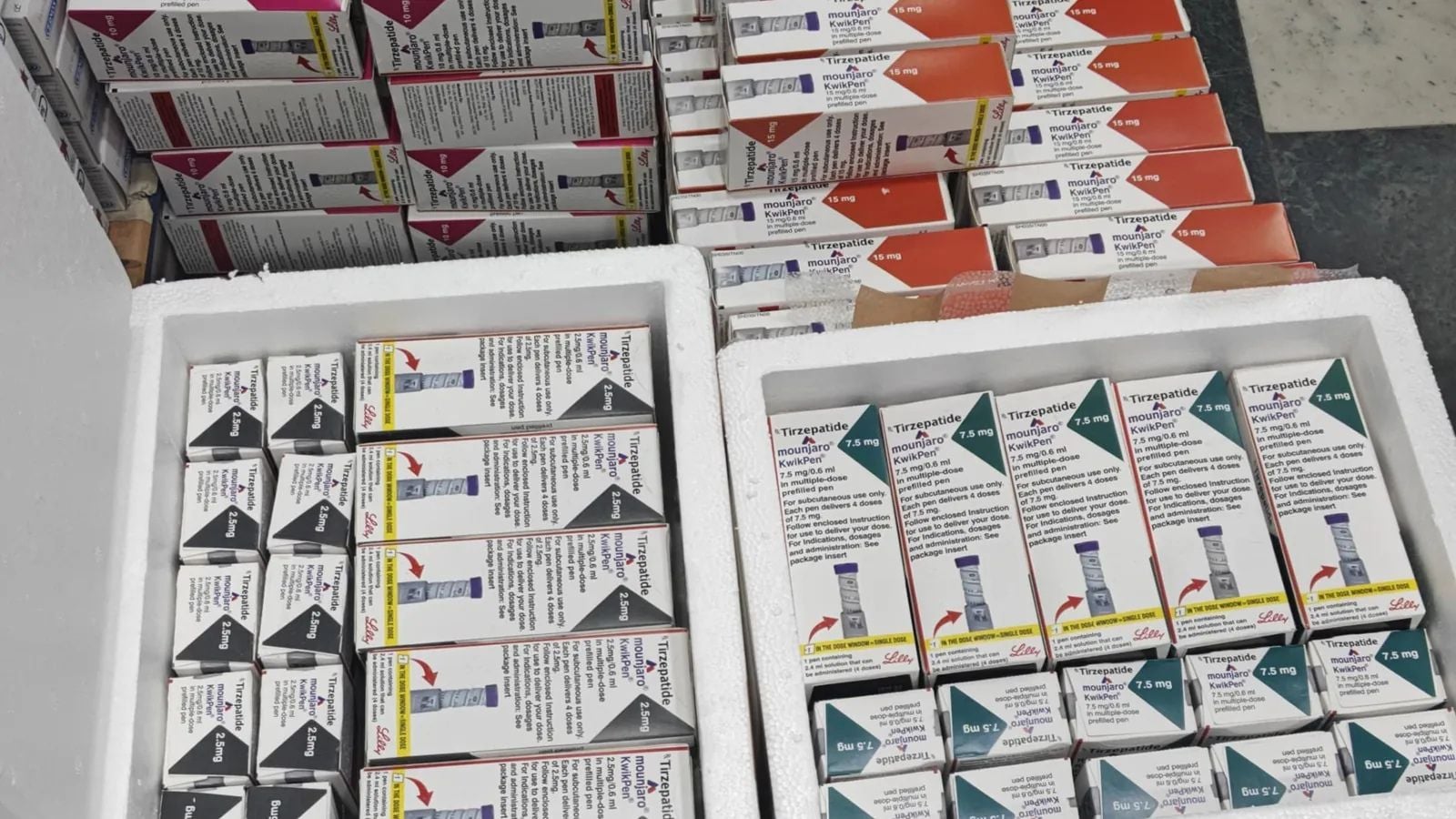
Then the seizure of counterfeit versions of Mounjaro KwikPen worth Rs 56 lakh in Gurugram exposed a racket that was manufacturing and selling the injections through illegal channels. That’s when he recalled a similar concern raised by another patient in Gurugram about two to three weeks earlier. “I had dismissed his fear too, assuring that the drug was internationally manufactured to high standards. But the recent case has introduced some doubt, making it harder for me to confidently reassure patients,” says Dr Misra.
So, he has sought clear guidance from regulators such as the Central Drugs Standard Control Organisation (CDSCO) on identifying genuine batches of the anti-obesity drug tirzepatide, warning that laxity would mean that patients would be at risk from counterfeit supplies.
In his recent post on X, Dr Misra wrote, “@CDSO (CDSCO) should clearly tell all of us who are prescribing Mounjaro how to identify fake batches.” Or else the efficacy of the drugs, which have been proven to control obesity and reduce risk factors of non-communicable diseases (NCDs), would be compromised. “I strongly urge the Government of India and CDSCO to issue a physician-facing advisory on identifying genuine tirzepatide — covering packaging, pen device features and supply chain verification — so that our patients receive full therapeutic benefits without harm,” he says.
Why an advisory is needed
Dr Misra feels that in the absence of an official advisory, doctors are left relying on unverified videos and social media discussions, which are not sufficient to establish authenticity. “If there is a clear advisory, we can identify it ourselves. Clinicians could also guide pharmacists and advise patients on how to check their medicines,” he adds.
Such clarity, he feels, is especially important, given the high costs of these drugs, which are challenging for patients, and the potential risks posed by counterfeit products.
Story continues below this ad
Dr Misra says that while the CDSCO has issued advisories on who is authorized to prescribe such drugs, a similar communication focused on identifying genuine batches would be useful. “Doctors would rely on and disseminate guidance that comes from credible government sources,” he says. He also cautions users against depending on information from AI tools or social media without verification, stressing that only authoritative guidance can resolve the confusion.
Why identifying fake drugs is difficult
According to Dr Ravindra Goswami, Professor of Endocrinology, AIIMS Delhi, identifying fake weight loss drugs is extremely difficult, even for doctors, because counterfeit products can look identical to genuine ones and are sometimes sold unknowingly through otherwise reputable pharmacies.
“Fake drugs are not a new problem and there have been earlier instances where even complex medicines, including biologics, were reportedly refilled into discarded bottles and resold, making detection very challenging. Because of this, simply issuing guidelines on visual identification may not be very effective,” he says.
Instead, he emphasises stronger enforcement. “Although laws and regulations already exist, they are not sufficient unless strictly implemented. The focus should be on cracking down on supply chains, tracing the source of such drugs, breaking criminal networks and ensuring strict policing. Those involved in selling fake medicines should face very severe punishment. Without strong deterrence, the problem will persist,” he adds.
Story continues below this ad
Dr Goswami also insists on strictness in ensuring the cold chain for drug storage. This is particularly critical for injectable anti-obesity drugs such as tirzepatide because they are temperature-sensitive biological molecules that need to be stored within a tightly regulated range, usually between 2°C and 8°C. Any break in this temperature-controlled supply chain — during transport, storage at warehouses, at the pharmacy, or even after purchase — can degrade the active compound, reducing its potency or rendering it ineffective. Unlike many conventional tablets, such degradation is often invisible: the pen may look intact, the liquid may appear normal, and there may be no obvious signs that the medicine has lost efficacy.
How counterfeit drugs impact patients
If the product is counterfeit, it may contain no active ingredient at all or even have contaminants. If it has been exposed to improper temperatures, it may become partially inactive while appearing genuine. In both situations, the patient may continue injecting it under the assumption that treatment is working, only to experience poor weight loss, unstable blood sugar control or unexpected side effects.
At one level, patients may simply fail to lose weight or achieve metabolic control, allowing obesity-related complications such as worsening diabetes, hypertension and fatty liver disease to progress unchecked. At another, counterfeit injectables may contain adulterants or incorrect concentrations that can trigger dangerous adverse effects ranging from severe nausea, vomiting and dehydration to allergic reactions, pancreatitis, electrolyte imbalance and kidney stress. In diabetic patients, ineffective or wrongly formulated medication can also lead to poor glycaemic control, exposing them to further health risks.
Patients who believe they are receiving an effective drug may delay seeking medical review when expected results do not appear, losing valuable treatment time. “Since these drugs work gradually and response varies from person to person, counterfeit or degraded products can remain undetected for weeks,” says Dr Misra.
Story continues below this ad
How many patients genuinely do not respond to drugs?
The number of non-responders is very low, according to Dr Goswami. “This could be because of poor response or drug resistance, which makes it even harder to definitively identify fake medicines based on outcomes alone.”